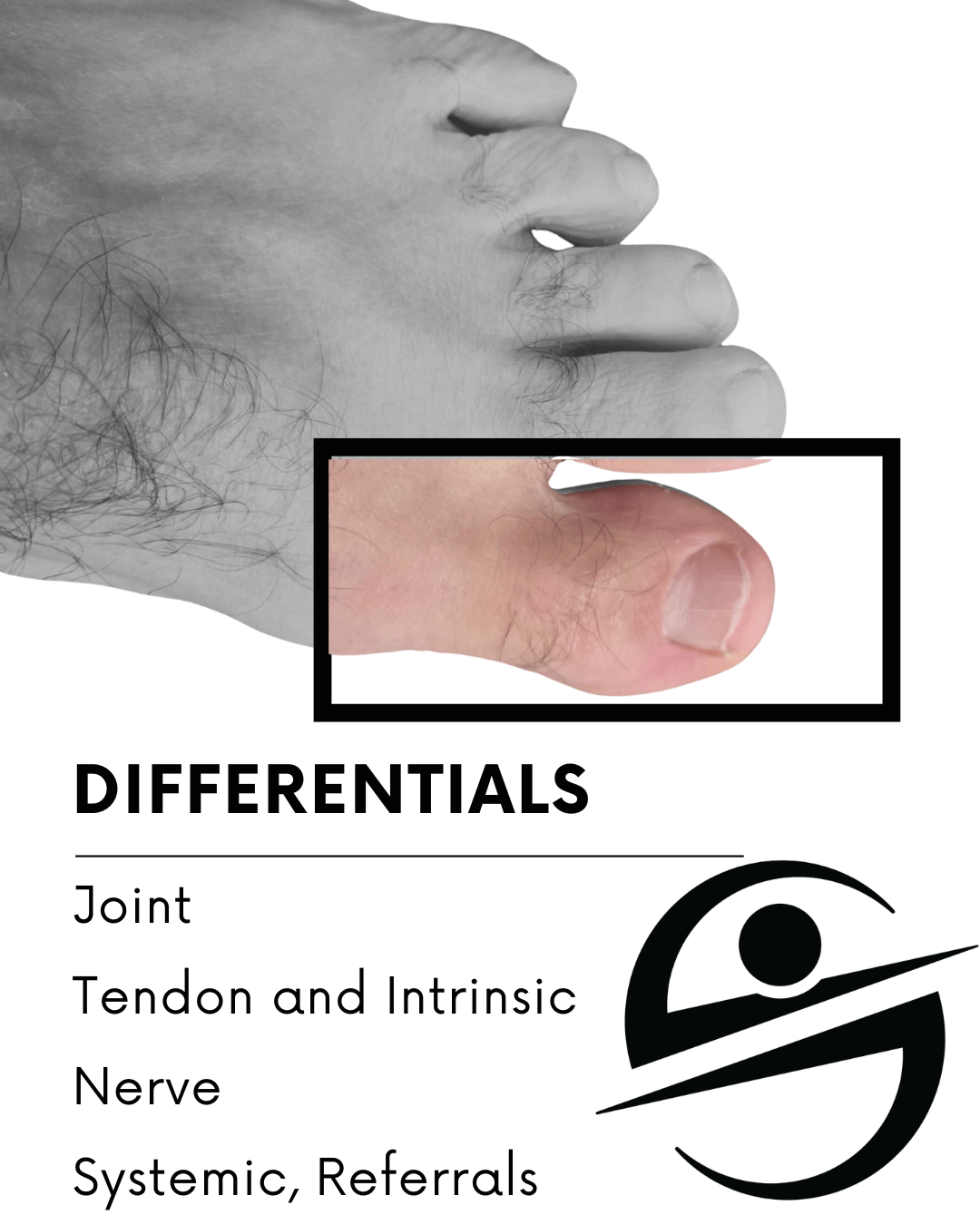
You cannot assume heel pain is from the plantar fascia — several other structures can be the true cause.
If you’re dealing with heel pain in Tucson that hasn’t improved despite treatment for plantar fasciitis, you’re not alone.
At Smith Performance Center, we often see people who’ve tried injections, stretching, shoe inserts, and ice bottles—yet their heel still hurts.
In many of these cases, the real problem isn’t the plantar fascia at all, but a muscle on the bottom of the foot called the flexor digitorum brevis.
You wake up, swing your legs to the edge of the bed, and… hesitate.
You know this is going to hurt.
The good foot moves to the ground first—you learned from that mistake a month ago. You brace and put down the other foot, the ungrateful one that will not get better despite the trip to the podiatrist, the injection, physical therapy, the shoe inserts, the ice bottle massage, and the stretching exercises.
The foot touches down.
It’s not so bad, you think, “those stretches and night socks are helping!”
Then you step—and the sharp pain feels as if the tissue from the back of the heel is ripping apart.
You think to yourself, “This plantar fasciitis won’t go away,” as you force your leg forward and take the next step and the next as the pain slowly reduces.
Diagnosing Heel Pain Correctly: It’s Not Always Plantar Fasciitis
As a general rule, you will be diagnosed with plantar fasciitis if you have heel pain. I have not seen a patient reporting heel pain that was diagnosed with anything other than plantar fasciitis for the last 5 years.
This is not the only structure on the bottom of the foot that can cause pain. Plantar fasciitis is not a common diagnosis in our clinic.
Your pain can be caused by any one or combination of the following:
- Flexor Digitorum Brevis
- Abductor Hallucis
- Abductor Digiti Minimi
- Fat Pad Trauma or Atrophy
- Stress fracture
- Lateral Plantar Nerve
- Medial Plantar Nerve
- Tarsal Tunnel Syndrome
- Low back referral
- Hip joint referral
- Plantar Fascia
- Surgical Scars
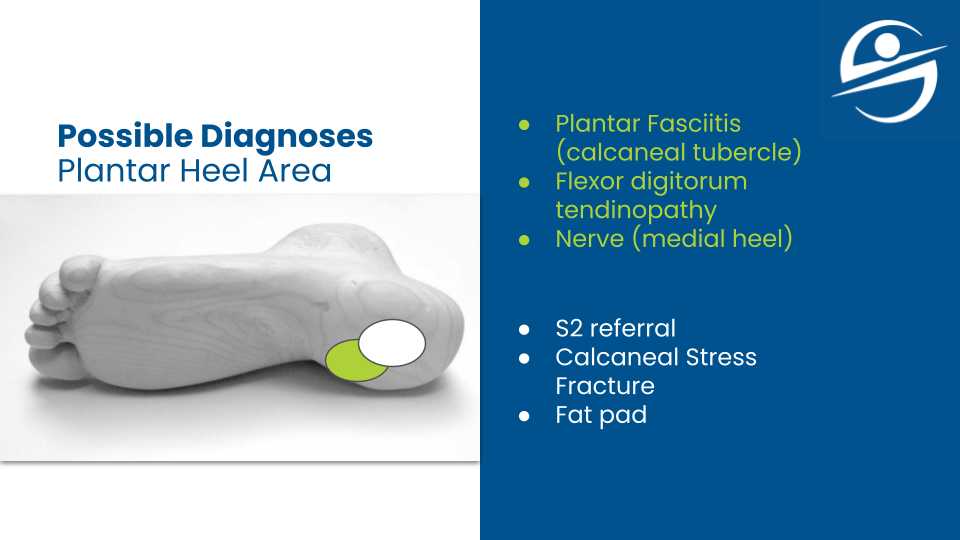
If you tried the treatments above and your heel pain is still there, maybe you don’t have plantar fasciitis. The flexor digitorum brevis is most likely the culprit.
If you are having pain in the big toe as well, you may be dealing with two different pain generators. Read our article Why Big Toe Pain Keeps Coming Back (and Why It’s So Hard to Fix)
Signs the flexor digitorum brevis muscle is causing your heel pain
What starts to clue you in that the pain is not plantar fasciitis but instead the flexor digitorum brevis or one of the other plantar foot muscles?
#1. Cramping on the bottom of the foot
The plantar fascia is not a muscle and should not cramp. If your foot cramps and causes pain, then it is highly unlikely that your plantar fascia is the problem. This is an important thing to catch in the medical history or subjective with the patient. Oftentimes, you may think it’s not cramping. Instead, it feels like the toes get stuck in a curled position.
Plantar muscle cramping is most common your ankle joint is plantar flexed and then the toes are flexed. With exercises, the most common one that causes foot cramping is the rearfoot elevated splits squats. The cramping foot placed on the bench will typically make the exercise unbearable.
If you sleep on your back at night, you may also get cramping from this position, especially with heavier blankets.
Other common activities include quad stretching if you hold onto the foot for the stretch, toe pointing in ballet, or sitting on your foot.
#2. Pain with resisted toe flexion
This is similar to the first sign. If you can induce heel pain or a cramp with resisted toe flexion, the flexor digitorum brevis is most likely the pain generator.
The initial physical exam can be negative for this finding, meaning there is no pain but after a cramp or loading with walking, resisted toe flexion becomes painful.
We also find that after several repetitions of the exam, a sore heel can develop while there is still no pain with the test.
I believe part of the issue with this is that the flexor digitorum brevis is used by the body as a local foot and ankle stabilizer, not a toe flexor, so resisted toe flexion does not provide enough load to the muscle to cause pain. The takeaway here is that you need to monitor pain after trying the resisted test and you may need to do it multiple times.
#3. Increased pain at midstance and initial heel rise
The flexor digitorum brevis supports the medial longitudinal arch of the foot. The muscle engages when your foot is flat on the ground. The plantar fascia is not loaded until preswing. You actually have more than a doubling in tension across the plantar fascia at preswing compared to the midstance and terminal stance.
The plantar fascia gets the most tension during preswing. This is due to a unique property of the fascia called the windlass mechanism. When the toe is dorsiflexed, the plantar fascia is pulled tight and pulled tight across the metatarsal heads.
A direct application of this means a shoe with a carbon plate would reduce the pain associated with plantar fasciitis but have no impact on a flexor digitorum brevis injury (the harder surface may actually irritate the flexor digitorum brevis).
#4. Flexor Digitorum Brevis Test
The flexor digitorum brevis and the plantar fascia have attachments by each on the calcaneus (the heel bone. They also run the same course on the foot from the heel to the toes.
A quick way to differentiate the two is to do the Flexor Digitorum Test.
Step 1. Tension the plantar fascia by dorsiflexing the toes
Step 2. Palpate the plantar fascia, especially the area that normally hurts
Step 3. Take the tension off the plantar fascia by plantarflexing the toes
Step 4. Palpate the same locations
If the pain is increased with the toes plantar flexed, your heel pain is coming from the flexor digitorum brevis.
#5. Pain or Cramping After Exercise
Many people with flexor digitorum brevis–related heel pain notice increased muscle cramping or tightness after activity rather than during it. This delayed response is a strong indicator of a motor control issue in the small plantar foot muscles.
When the physical exam is negative in the clinic, we often ask patients to perform their usual activity—such as running or lifting—and then retest. After loading the foot, resisted toe flexion often becomes painful, and the muscle cramps more easily.
At Smith Performance Center, we frequently analyze these post-exercise patterns through a running gait assessment to confirm whether the flexor digitorum brevis is the true source of heel pain.
#6. Holes in your footbed
If you pull out the footbed from your shoes, you may notice indentations where your toes normally push down. If the indentations are deep (sometimes there is actually a hole in the footbed where the big toe push down) then you are likely burying your toes during the day and with walking.
When you bury your toes, it’s often a sign of weakness in your plantar flexor muscles or an issue with balance, or both. The problem is that this overloads and irritates the flexor digitorum brevis over time.
You may notice blisters on the end of the toes. This can be the same process happening as well.
#7. Abnormal walking style (gait)
When the flexor digitorum brevis is irritated, people often shorten their stride to reduce time on the painful foot—especially during midstance, when the muscle is most active.
By contrast, someone with plantar fasciitis usually avoids the toe rocker phase at the end of gait to reduce tension on the plantar fascia. This small change creates a distinctive walking pattern that an experienced physical therapist can easily recognize.
Understanding when and where your foot hurts during walking offers key diagnostic clues about which structure—muscle, fascia, or nerve—is responsible for your heel pain.
Flexor Digitorum Pain: These Signs Do Not Mean It Is Plantar Fascia
Morning pain
The presence of morning pain does not differentiate between plantar fasciitis and plantar muscle tendinopathy. Both injuries commonly have this report. With tissue that has chronic inflammation, more stiffness, and discomfort are common after a period of rest.
Pain worse with the initial loading
This is another one that does not differentiate between plantar fasciitis and the muscle. A common report is that walking or running feels terrible but then gets better.
Flexor Digitorum Brevis Pain Versus Plantar Fasciitis Pain
The first step in treating heel pain is understanding the pain generator.
The most commonly used criteria to diagnose plantar fasciitis does not differentiate between the flexor digitorum brevis and the plantar fascia. If you have one or more of the signs or have been trying the normal suggestions for treatment without improvement, then the flexor digitorum brevis might be the culprit.
If that is the case, then there are other things to consider.
If you currently have heel pain, check out our article “4 Ways Individuals With Heel Pain Can Make Their Pain Go Away“
Do you want to understand what is causing your symptoms?
If you have been dealing with pain or injury that does not seem to be getting better and no one determined what is causing your pain, we can help.
You can learn more about our Physical Therapy Services or schedule a Physical Therapy Initial Evaluation and start walking pain free.
References
- Chen Y-N, Chang C-W, Li C-T, Chang C-H, Lin C-F. Finite Element Analysis of Plantar Fascia During Walking: A Quasi-static Simulation. Foot & Ankle International. Published online September 4, 2014. doi:10.1177/1071100714549189