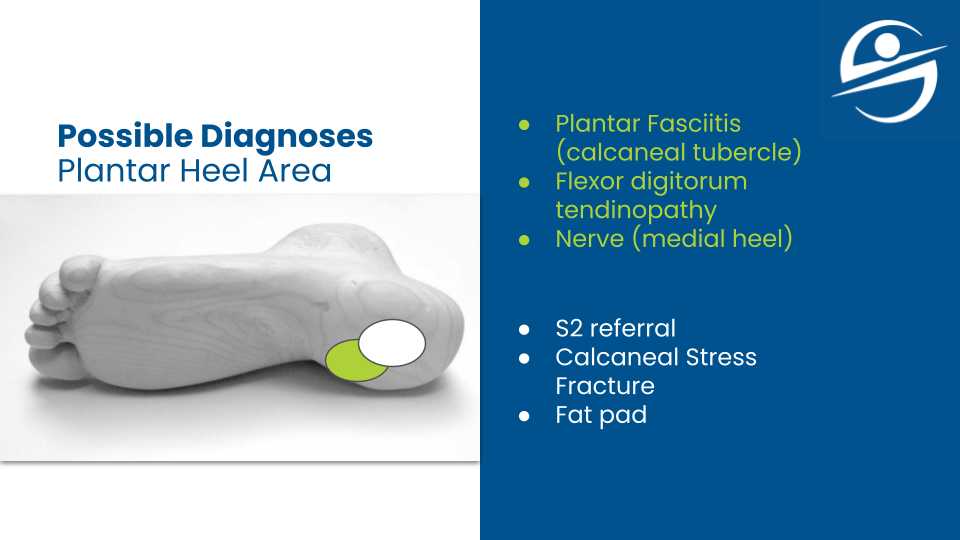
How do you manage knee pain with a meniscus tear?
Meniscectomy, sham surgery, and clinical experience avoiding surgery for pain and function
Clinical practice is filled with successes and failures. For some reason, the failures are the thing you remember most and for me, lead to the biggest changes in practice. The patient that never feels better will never quite leave your mind even when you go home from work.
Knee pain and Meniscus Tear – Round 1
Since my main interest has always been the lower extremity, specifically the foot, ankle, and knee pathomechanics and pathology, I wanted to be the best at rehabbing these injuries right off the bat. My failure with a patient suffering from chronic knee pain led me to the literature surrounding meniscal surgery. The patient reported sharp pain with occasionally catching in the knee joint. The joint had mild joint effusion and full knee motion with pain at the end ranges. The most pain was end-range knee extension. The patellar tendon was exquisitely (love this word) tender. She walked with excessive knee extension at loading response into midstance.
We started physical therapy with a focus on the patellar tendon and at that time I used way too many quad and glute exercises without focusing on the clear issue of walking and joint irritation.
The patient would get better, then worse, then better, then worse. The cycle repeated over and over and over. Finally, she was tired of the pain. I learned a lesson that my current thought process was dominated by managing a patellar tendinopathy when something else was clearly occurring.
She was diagnosed with a degenerative medial meniscus tear and had surgery. The presence of the meniscus and knee pain meant that the tear had to be the cause of the pain – which is not necessarily true. I remember talking with her when she said all the pain was from the meniscus. I saw her for rehab after the procedure. She got better and I discharged the case.
Knee pain and Meniscus Tear – Round 2
A couple years later the pain returned. The presentation was similar, however, my focus changed from addressing the returned tendinopathy to fixing the walking gait and improving the joint related pain. She also happened to get imaging and was considering another meniscectomy due to further meniscus degeneration.
The difference in treatment was considerable.
We focused on meniscus mobs and knee extension. When we got a pain-free extension and the quad firing normally, her walking was pain-free. However, it did return to normal and she kept returning to her excessive knee extension pattern. After doing specific practice on this, she started to use it without cuing and all of the pain resolved.
My change in practice occurred for two reasons:
Analyzing the poor outcome
I was missing something in the presentation and in my feedback loop for the treatment
I kept doing the same thing without good results
I ignored part of the exam and focused on one area when two pathologies were clearly present
I ignored the walking abnormality that was most likely the functional cause of all of her symptoms.
Research shows no difference between sham surgery and partial meniscectomy
There have now been several papers that have shown no difference between a partial meniscectomy and sham surgery, but the first was in 2013.
Sihvonen R, Paavola M, Malmivaara A, et al. Arthroscopic Partial Meniscectomy versus Sham Surgery for a Degenerative Meniscal Tear. New England Journal of Medicine [Internet] 2013 [cited 2020 Sep 1];369(26):2515–24.
The authors decided to do the study after another study compared meniscectomy with physical therapy to physical therapy alone and there was no difference in outcomes.
They did a great job blinding the participants:
The patients who signed up were told they could either get a sham surgery or partial meniscectomy
The surgeon did not know which procedure would be conducted until the operating room when they opened up the envelope with random designation determined by the statistician
If there was a sham surgery, the surgeon took the same amount of time, made the incision, and moved the leg around simulating the procedure.
When they analyzed and started to write up the outcomes, the data was blinded:
“treatment A (results) compared with treatment B (results)… assuming that treatment A was arthroscopic partial meniscectomy, and the other assuming that treatment A was sham surgery.
After the authors agreed on the analysis, the code was broken so the actual treatment performed was known.
No difference was found between the two groups. They concluded that..” results argue against the current practice of performing arthroscopic partial meniscectomy in patients with a degenerative meniscal tear.”
From this experience and this research, a big takeaway is that when the degenerative process is happening, we need to search for the root cause and problem. We cannot do a procedure and think that this is the only issue. It is just fixing a symptom. For better long-term outcomes, we have to consider more. If you have knee pain and a meniscus tear, there are physical exam tests to figure out if it is causing the pain. This includes effusion in the joint, painful passive end-range extension, and special tests for an anterior horn meniscal lesion. If you have these findings, you can use them to retest and make sure the physical therapy plan is working and prevent a surgery that does not appear to do what most people think.
Other articles on the knee
Physical Therapy Solutions for Knee Pain
Arthroscopic Partial Meniscectomy Surgery Vs Sham Surgery
Factors To Consider In Returning to Play
Physical Therapy Research: Update On The Knee And The Brain
Tuck Jump Assessment
Physical Therapy Exercises
Partner and Self Traction
Bracing, Taping, and Training Aids